At what point is addressing sterile field control overkill? I mean, on one hand it’s never a bad thing per se, but in a cost-competitive world, lines have to be drawn somewhere or you’ll lose money providing protections that are redundant. Should one always strive to be better? Or does one reach a level of risk mitigation where no reasonable improvement is left to be had, and it’s better to move on to other areas?
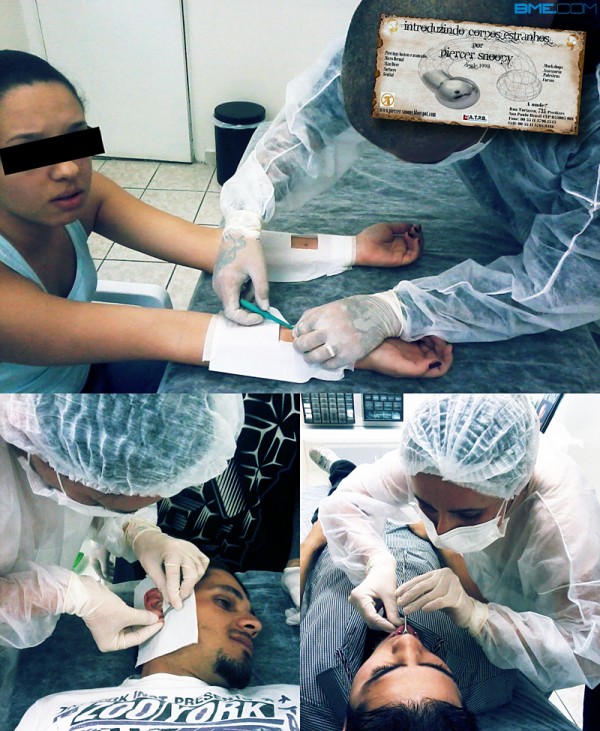
I’m really blown away (in a good way) by the level of concern Ronaldo “Piercer Snoopy” Sampaio of Sao Paulo, Brazil (piercer-snoopy.blogspot.com) pays to even “basic” procedures like navel piercings, wearing full surgical gowns and a mask in addition to the industry standard gloves. We all accept that gloves are needed. This is not so much to avoid skin-on-skin contact between the piercer and their client, but because changing gloves is the easiest way to control cross-contamination. Oversimplifying the matter, the primary purpose of gloves is to provide a barrier between clients (even though they’re rarely in the room at the same time), to stop transmission of blood-borne diseases from one client to the next. Gowns, hair nets, and masks on the other hand primarily provide a barrier between the piercer and client. In addition to these protections, in some cases this studio does the procedure through a “window” in a surgical drape. In addition to creating psychological clarity by isolating the procedure from the rest of the environment, this minimizes the risk of pulling any bacteria from the surface of the client’s skin into the wound.
On one hand, all of these protections reduce the chance of infection and related complications as well as projecting an air of professionalism. But on the other hand, humans have been piercing each other with dirty sticks in caves for perhaps the last hundred thousand years. What do you think? Where do you draw the line for acceptable minimum standards? What do you expect of a top-notch shop? Is there a level where you begin questioning the allocation of resources? Do different procedures have different rules? No matter where you think the line should be drawn, I hope you agree it’s wonderful that people are working at such a high standard to even allow such questions to be asked!
 BME/News and Modblog highlight only a small fraction of what
BME/News and Modblog highlight only a small fraction of what
In a surgical room, the whole place is sterile. In a tattoo/piercing studio, when everything else is not sterile, it is too much and only for the clients’ eyes. The clients have microbes on them, on their clothes, and the room as well can never be as a surgical room. They walk with shoes on.
I have had consulted a doctor once about the importance of wearing sterile gloves instead of regular gloves from the box. He simply replied to me that if the room is not sterilized, everything that was sterile seises to be the moment we open it.
That’s the story.
It is eye candy for a client to see a very clean piercer, but that’s all. If a piercer keeps the standards, it’s up to the client to follow the instructions afterwards, and this is most of the times the problem.
It’s an interesting question of balance. I just had to make some decisions along those lines while mixing some electrolyte for a customer’s large off-grid battery system. When handling the pure potassium hydroxide powder, I was wearing a gown, heavy-gauge gloves taped to the sleeves to prevent intrusion, a NIOSH breathing mask, and a full-face shield. The powder will react with skin moisture and can start burning into you quite quickly (go watch Fight Club for an idea of what that might look like).
Once it was mixed to a 25% solution, it’s still quite dangerous, but you’ll likely have time to run over to the handy jug of vinegar (always have a handy jug of vinegar when working with stong bases) to douse the affected area. So, at that point, I removed the breathing mask, replaced the heavy-gauge gloves with standard nitrile exam gloves, and didn’t bother to tape them. Trying to work while wearing all that would have actually made things less safe, by increasing the probability of a spill.
The moral of the story is that you need to balance the theoretical safety offered by a given technique, with the chance that the technique in question will degrade your ability to perform. If you have so many layers of protection in place that you are actually performing sub-par piercings as a result, that would be a definite point at which to take a step back. Does using a sterile drape increase the risk that a piercing will be put in crooked, because the piercer cannot take cues from the nearby anatomy? If you wear a face shield and surgical mask, does that impede your ability to see what you’re doing, to a greater extent than it protects the client from a sneeze, or you from the client’s blood?
Good evening friends of BME! First would like to present! My name name is Ronaldo Sampaio will work as a Professional Piercer 15 years in Brazil for six years and was executive vice president of the Union of sp-Setap Tattooists and Piercers Brazil. Currently coordinate classes focused on technical and technological education alongside other greats such activity throughout Latin America. I let them know that here in Brazil such attire is mandatory for all who work in the practice of Body Piercing and Tattoo. We create a bill with the Federal Council of Medicine even when the entity class was composed. I firmly believe that today with this range of people making such maneuvers the differential should be employed not by exaggeration, but considering the viral and bacterial mutation on the planet. We got our freedom in 2007 along with professional health agency so that my parents can make use of punch biopsy and catheters because such maneuvers are not aiming prognosis or diagnosis. I have contact with people of APP which helped me last year to do a Educational Congress for Piercers South American extension of Professional Piercers Association. Some punches in Latin America still has difficulty getting material taken as themselves in this industry … Like for instance jewelry screw reverse, so that umj great friend Atacama Chile – Known as Mauricio Torres began developing jewelry within the rules of the Association for facilitate our acquisition. We are currently using the perforations in first Titanium metal – certified (Ti6Al4V ELI) that is ASTM F-136 compliant or ISO 5832-3 compliant, or commercially pure titanium, which is ASTM F-67 accordingly.
Fico feliz Sannon pela sua observação em relação e deixo aqui registrado o imenso respeito que tenho pela sua pessoa. Enfrentamos atualmente uma intervenção dos órgãos de saude referente a pratica do Implante 3D, Bifurcação Lingual e Transdermal o qual buscando legislações sobre esta pratica no mundo, descobri que a maioria dos paises também adotaram tal postura em relação.
Estou fundando a Associção dos Tatuadores e Piercers do Brasil com o intuito de resguardar os nossos direitos e deveres. Companherismo , Ética e Respeito palavras chave para a difusão segura e adequada de tais pratica nos dias de hoje!
Cordialmente.
Ronaldo Sampaio – Piercer Snoopy.
I’m using google translator forgive me for my linguistic handicap! When we exercise this activity with such dedication language barrier is just a detail!
I commend fellow body artists for application of sterile barrier precautions and measures to protect themselves and their clients.
It is easy to concede that it seems that a body artist can get away with less precautions during a procedure.
The bandwagon fallacy is not an acceptable argument in the case of a commercial elective procedure.
Overkill is the definition of what we do when we sterilize a needle and other equipment used for a margin of safety, since sterilization is a matter of probability, and not a perfect process. Sterile instruments, sterile gloves masks and the appropriate barriers proven in clinical practice to maintain asepsis make a measurable difference in the infection rate. We should not have to rely upon the assumption that each client has a healthy immune system fully capable to fight of MRSA, M. chelonae, C. difficile, HCV or any of the other pathogens that could be spread through contact during a service. Assuming that clients can handle exposure and weighing this against expense leaves much to risk in for the service provider in this business.
It is not necessary to strain to make weak comparisons to ancient piercings done without asepsis with thorns etc. We don’t live in those days, and can’t draw a valid comparison. Think of how far we have come since then with sanitation, soap, clean water and sewage treatment, and the knowledge of antisepsis and asepsis. http://brnskll.com/shares/a-brief-history-of-sterilization/
I can state clearly that sterile barrier precautions should not impede the speed or accuracy of a procedure. Masks, eyewear, drapes etc improve the process when used appropriately. Every tool requires training to handle correctly, and these barriers are tools that should be used with care, just like a needle. Furthermore they should be learned before working with a sharp instrument.
In Sr. Sampaio’s case, he follows the specifics of the Brazilian safety regulations with care, negotiated to prevent the enactment of draconian regulations in his region, and shares this information openly with colleagues.
I see this as a positive article that could encourage many body artist to try modern safety precautions for their client. Please stop questioning the validity of safety precautions and start trying them out. Learn more about them from professionals who use them correctly. I find modern safety measures fun to learn and to apply to procedures. Here is an example: http://brnskll.com/shares/dental-bib-vs-sterile-drape/
In community,
Brian Skellie
Well it’s not necessarily bad to have the best protection you can get however, being in the client’s position…I would feel terribly uncomfortable in a “procedure” like that. I like to see the person who’s piercing/tattooing me and their reactions/emotions/charisma/etc. I feel like maybe this sort of safety could cause an emotional “barrier” between the client and the proffessional. I guess that’s not necessarily a bad thing but to me the whole surgical procedure and doctor look feels “cold” to me.
I’ve never liked doctors though so maybe I have a little bias… The whole medical world sort of intimidates me and drives me nervous for no reason!
I’m with Claudia. This kind of setup would put me off. It’s far too clinical and cold seeming, and I’d feel more like I was at the dentists or something done than being pierced. I’m quite a nervy person so I like being able to see people’s faces when they’re going to pierce me. To me, this seems more about protecting the piercer than the client, as you said, people have been piercing each other with sticks for thousands of years and most of them survived.
I like your comment that people have been piercing each other for centuries with dirty sticks. It makes a pretty valid point about how much is too much. There are no auto claves out in the African savanah or the South American rain forests yet some of the people there still continue to this day a tradition of body modification with more or less no ill effects.
I am not advocating going to a dirty shop or having procedures done with an old rusty needle, but just because a shop doesn’t spray down everything with bleach or a disinfectant wipe after every single time the practitioner touches something, that doesn’t make it an unsafe shop.
@Claudia and Ellie: A still photo of these procedures goes a long way at dehumanizing the body mod artist by removing the warmth and kindness of their gestures, expressions and voice. I use similar precautions and they by no means impede a conscientious, fun and friendly relationship between my clients and me. The main interactions are outside the procedure room, and when it comes to the moment of truth, scrubbing in and suiting up is quick, and I can maintain a conversation the whole time, while introducing and explaining each precaution as desired to familiarize my clients as I go. It is a build up, you are not presented with a scary dude in a smock and face mask the moment you walk in the studio.
@Anthony:
1. The apologist conjecture that people have gotten away with less safe mods in situations where safety precautions were not available is not a valid comparison as I stated before, and does not make it an acceptable practice *in a commercial setting.*
Due diligence will show that sterile barrier precautions have been proven to save lives in clinical application, and therefore will be useful to protect them for body mod procedures. The wishful thinking of “more or less no ill effects” is a fallacy projecting hopes for the ideal “Noble savage” on people who have a very different scenario than what we experience in a studio setting.
2. Lack of proper cleaning, disinfection and sterilization (in that order) does make for an unsafe shop.
What you seem to ridicule is the professional application of chemicals for hard surface disinfection, which I agree seems pretty silly without first cleaning the contaminated surfaces, and seems unnecessary to do if the procedure was properly contained to the insides of sterile barrier systems. The outside barriers keep the inside sterile when handled and opened correctly. Most procedures can be done with very minor mess, and that can be kept inside the barriers and disposed of.
For example, what I use for a procedure is sealed until the moment before use in an impervious sterilized metal container or other sterile barrier system, so the surface underneath that container needs only be cleaned and dusted and occasionally disinfected, but not necessarily sterilized unless there was a spill or splash. The client seating area should be cleaned and disinfected between each procedure, but that is the only area in the room that frequently gets contaminated with anything beyond minor airborne particles, thus cleaning and dusting and occasional disinfection suffice. Some would disinfect all horizontal surfaces anyway, just in case.
The important part to take away from this is that very real safety issues involving life threatening and very unpleasant pathogens have to be addressed in modern commercial application of body art. Safe procedures can still be fun, quick, accurate and above all else a valuable human experience.
Further discussion to help clarify this here:
https://www.facebook.com/brian.skellie/posts/283356151773006
Yes, people have been piercing each other in caves with sticks, yadda yadda. But those piercings were very risky, and could lead to infection and death. The need for complex aftercare meant that not everyone could have them, and back then, we didn’t have MRSA.
I think that for a simple surface piercing, though, a surgical gown is overkill, purely to impress the client. As pointed out above, a surgical theatre is a sterile environment, and that is reasonable for surgery deeply penetrating the body. I have actually had doctors perform simple, superficial surgeries on me without gowns, sterile fields, etc. They aren’t needed for a piercing.
I agree with Faye in the first post. The room is not sterile, the client is not sterile and still wearing their street clothes. Gloves mandatory, plastic disposable apron as an ideal addition. I do question the material of the additional protective gear, and couch cover, is it thin and porous cotton, like disposable underwear ?
Mire aca Amigos!
http://www.daltonsilvano.com.br/leis/ver.php?id=56
@Faye: that doctor was very much wrong about things ceasing to be sterile by being used in a non-sterile room.
The purpose of a sterile field is to create a sterile area in which to work, even if the room is not sterile.
Statistically-speaking, the majority of surgical procedures are almost certainly performed in emergency rooms, which are non-sterile.
@ Flint- and that’s why in hospitals and emergency rooms they open a sterile wound care pack for each patient. My point is they open a new sterile pack, it’s not just a clean item pulled from an open box.
Wound care packs contain something like a pair of gloves, 2 plastic backed surface covers,1 plastic apron, 5 squares of gauze, tray for sterile washing liquid and large bag to dispose of the contaminated soft stuff – I use these in my work, they cost about 65p each. Of course I go thru more gloves.
For the service I offer (cosmetic tattooing) I consider not using individually wrapped sterile gloves each and every time an acceptable risk – I’ve always got clean hands when I handle the glove box so it’s not cross contaminated, but it isn’t sterile.
Individually wrapped sterile gloves are put on differently to keep them sterile on the outside, the cuffs are already rolled down so you don’t need to touch the outside to put them on.
this is an interesting debate . i have had procedures that are more invasive then a piercing done with much less precautions and drapes .
@Brian Skellie. I am not ridiculing being proffesional and clean, but there comes a point when enough is enough. From what you described, you follow a pretty similar procedure to what I have experienced in most shops. That is a good thing. I have been in a shop where overkill was the word of the day.
I was reffering to a shop I went to one time, and only one time that took over an hour to do my nipple. First the piercer but on gloves,then wiped the gloves down with a bleach wipe, then opened the can with the toothpics, marked the piercing and discarded the toothpic. Once he had put the lid back on the can the whole table and the can got doused in bleach spray, then a glove change, another wipe down of the gloves with bleach and he got the pertoleum jelly to lube the needle out of the jar with a tounge depressor. Then the table and all the containers got doused in bleach again. Then the 3rd glove change and wipe down of his gloves with a bleach wipe. Then he took the needle out of a drawer in the table, set it down and the whole process started again. By the time it was all done he had changed gloves 5 or 6 times and all I could smell was bleach. It took so long and was such a pain that I won’t got back to him,ever.
@Lisa: indeed. Using sterile, pre-packed supplies can achieve the desired result, even in a non-sterile room.
I disagree with some comments:
I do not think that the use of a perforated sterile field means less accuracy, by contrast, we can rely on the
client better without polluting our gloves.
I also disagree with not using sterile gloves, because they are contaminated when opened, is a cheap excuse and baseless.
also the sterilize the jewelry, and when opened becomes contaminated, but it depends on our procedures and our ability to perform work in the best conditions, preventing cross contamination.
my respects to all and sorry not speak English.
use sterile gloves and would never let someone put a piercing my children with non sterile examination gloves.
Last thing, the customer is not sterile, the room either, but the tissues under the skin are sterile, so the needle should be, the jewel too, and we wear gloves too. if you do not want to use sterile, because no interest is not because it is necessary.
Note: These precautions are mandatory, as Sr Sampaio linked above: [A translation]
“Article 5 The professionals that run the processes of tattooing, permanent makeup and fixing “piercings” as well as his assistants, must use clean aprons, masks and gloves and disposable single-use goggles.”
These are not sterile surgeons gowns, simply a clean single use apron, as required in California, for example. The hair cover and mask are likely to make a greater difference as far as the professional’s attire.
The sterile barrier precautions and accurate application of asepsis with sterile gloves, sterile drapes and all sterilized instruments and jewelry are the critical safety elements that set this procedure apart from those done with non-sterile measures.
It is not valid to compare elective cosmetic procedures to emergency procedures in terms of safety precautions. The former has the opportunity for controlled asepsis on a clean subject, and the latter requires antisepsis as well as asepsis to /treat/ and prevent infection, and is outside of what body artists without medical degrees and licenses can do legally.
I agree with the statements made by @Flint, which demonstrate understanding of modern asepsis.
@Lisa, perhaps you could consider sterile gloves as well, and working with an aseptic rather than clean procedure? Many tattoo procedures can be done with sterile barrier precautions effectively. I notice that the tattooist’s perspective tends to be similar to dental hygiene “sterilize before use,” rather than dental or medical surgery “maintain sterile until and during any contact with the subject,” which is encouraged whenever possible. New, unopened non-sterile exam glove boxes have been found to contain Mycobacterium and other microorganisms, so to be safe it is prudent to at least use items that are sterilized before use.
@Anthony, the shop procedures you describe would be what I consider “faking it.” This scenario shows that the practitioner did not understand asepsis, and attempted to make up for it with antisepsis. You are correct to call that out as an inappropriate misinterpretation of safety. Non sterile exam gloves are not meant to be wiped down with chemical disinfectants, and are not usually improved by doing so. With all that chemical effort, the procedure was still likely contaminated from the bulk petroleum jelly, the non-sterile work surfaces that the needle was introduced to, and the overall lack of sterile barrier precautions,
Just to clarify you do not and could not sterilize an operating room. Ive been piercing for 12 years and also spent the past 2.5 years working in an operating room assisting surgeons in surgical procedures. While i dont feel the need to wear all the ppe mentioned i do still feel that draping masks and sterile gloves are appropriate for the procedures we offer in a studio.